
Pictured left to right: Jack Doyle Taylor, Dr Brian Keogh, Lise Alford (3ts), Joe Loughnane, Professor Louise Doyle, Committee Cathaoirleach Deputy Louise O’Reilly TD, Albert Dolan TD, Pat Buckley TD and Louis O’Hara TD.
On Tuesday, 24 February Joe Loughnane, Advocate, Adam’s Protocols Campaigns, and Professor Louise Doyle, Head of Mental Health Nursing, Trinity College Dublin, presented powerful witness statements to the Joint Committee on Public Petitions and the Ombudsmen on the urgent need to establish Mental Health A&Es and 24/7 Crisis Care Centres in Ireland.
Joe spoke to the committee about his belief that his brother, Adam Loughnane, would still be alive if such centres of care had been in place when he sought help.
To date Joe has gathered over 22,000 signatures on an online petition in Adam’s memory, campaigning for the establishment of Mental Health A&Es.
Professor Louise Doyle outlined key service recommendations originating from research studies conducted by Trinity College Dublin, funded by the 3ts Charity (Turn the Tide of Suicide) and the Irish Research Council (IRC).
Key service recommendations:
- Increase the range of unscheduled and crisis mental health services in the community for those presenting with self-harm, suicide-related ideation and suicide attempt.
- Both service users and accompanying family members repeatedly called for alternatives to the Emergency Department, or sub-units of the Emergency Department, providing safe, calm, specialised mental health crisis centres staffed by mental health professionals.
- Increase the capacity of community mental health teams to respond to urgent referrals of new and existing patients.
- Targeted investment in Child and Adolescent Mental Health Services, particularly for emergency presentation to prevent children and adolescents being held for long periods in adult ED environments.
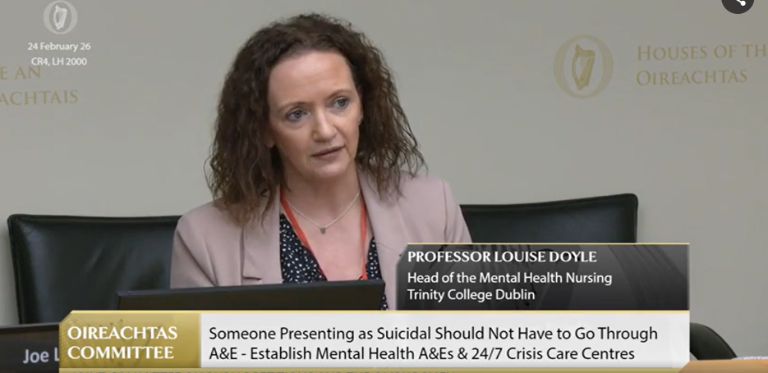
Professor Doyle (pictured above) said in her opening statement:
“The Emergency Department will always be part of the mental health crisis landscape. But it should not be the only door and, crucially, when people do walk through that door, the experience must be safe, compassionate, and responsive.
For some in our studies, this was the experience, particularly when seen by specialist mental health staff including those working as part of the National Clinical Programme for Self-Harm and Suicide-Related Ideation.
However, for many, the healthcare responses in the Emergency Department were sub-optimal. Our studies show that people in suicidal crisis, and their supporting families, are not asking for complex interventions in an emergency setting.
They are asking to be treated with dignity, listened to with patience, and supported with care in an appropriate environment.”

/filters:quality(100)/prod01/channel_3/media/tcd/nursing-midwifery/images/news-images/Irish-Times-Logo.png)
/filters:quality(100)/prod01/channel_3/media/tcd/nursing-midwifery/images/news-images/Irish-examiner-1.jpg)